Defaut de cartilage ou pathologie ostéochondrale de la cheville
Définition
La mobilité entre deux os est possible grâce à une surface de glissement qui est appelée « cartilage ». Au niveau du pied et de la cheville, son épaisseur est environ de quelques millimètres. Afin d’améliorer le glissement de ces surfaces cartilagineuses, la capsule articulaire fabrique un liquide appelé « liquide synovial ». On peut définir un défaut ostéochondral comme une interruption de cette surface articulaire qui atteint le cartilage mais aussi l’os sous-jacent. Dans cette région, ce kyste est considéré comme une cavité remplie de liquide articulaire.
Causes et symptômes
Des entorses et des fractures peuvent évoluer vers des lésions du cartilage. Dépendamment de la direction, de la rotation et de l’intensité des forces ayant eu lieu lors du traumatisme, la lésion de cartilage peu évoluer de la simple déchirure à la fracture déplacée ou non, associant parfois une partie de l’os sous-jacent et restant attachée au cartilage.
Une simple déchirure peut passer inaperçu et guérir spontanément, à votre insu. Cependant suite à la pression dans l’articulation, le liquide articulaire peut s’insinuer dans cette fissure et crée, petit à petit, un trou liquidien dans l’os (kyste ostéochondrale), juste en- dessous du cartilage. Dès lors, vous pouvez ressentir trois types de plaintes, parfois associées entre elles.
- Une douleur profonde dans l’articulation, secondaire à l’excès de pression:Suite à l’augmentation de pression en station debout ou lors de la marche, la pression augmente dans l’espace liquidien du kyste ostéochondral.. Comme il existe des nerfs sensitifs en région sous chondrale, la douleur est perçue et augmente.
- Sensation de blocage:Parfois, avec le temps, une partie du cartilage qui était stable c’est partiellement détachée. Par ce phénomène, cette partie peut se tourner et bouger lors de certain mouvement et crée la situation comme si quelque chose se bloque lors d’un mouvement normal ou comme si quelque chose se déplace.
- Instabilité: Certains patients souffrent, après une entorse de cheville par exemple, d’une instabilité, accompagnée d’une douleur. Souvent provoquée par une déchirure des ligaments péri-articulaires ou par la présence d’une lésion cartilagineuse. Lorsque certains mouvements provoquent une douleur, on ressent une instabilité subjective. En fonction de la localisation, de l’intensité de la lésion, de votre âge et des traitements antérieurs, de multiples interventions peuvent être proposées
Traitement
- Débridement arthroscopique et microfracture
Par deux petites incisions on explore, et on traite à l’aide d’une caméra et d’instruments adaptés, la lésion cartilagineuse ce qui permet une réduction de pression. Dans la littérature, cette intervention a un pourcentage de réussite de 60%. Cependant en perçant de petits trous dans l’os sous-jacent (microfracture), on apporte une meilleure circulation sanguine et le taux de succès passe alors à 85%. Après l’intervention, on met un pansement compressif pendant 3 jours car il faut bouger la cheville rapidement. Cependant, il est absolument interdit de s’appuyer sur cette cheville pendant 6 semaines pour permettre à l’hématome de se transformer partiellement en os et partiellement en une nouvelle surface cartilagineuse qui doit s’attacher à l’os et au cartilage périphérique. En s’appuyant, par les effets de pression, le liquide articulaire « lave « le caillot sanguin et empêche ce phénomène de réparation cartilagineux.
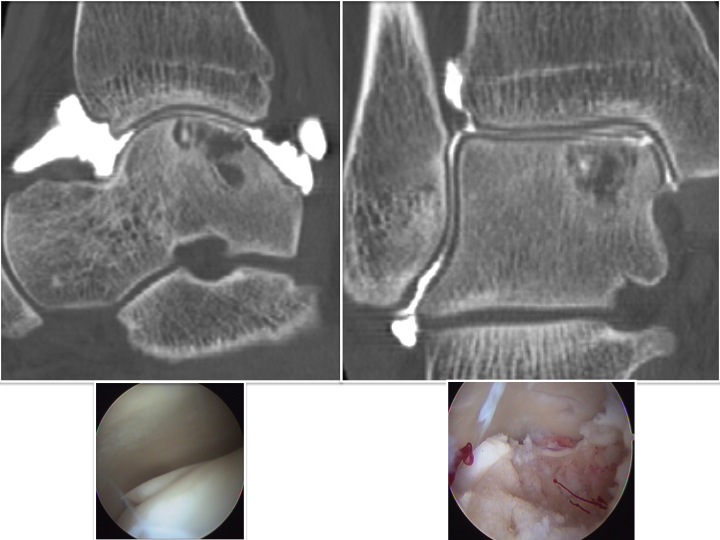
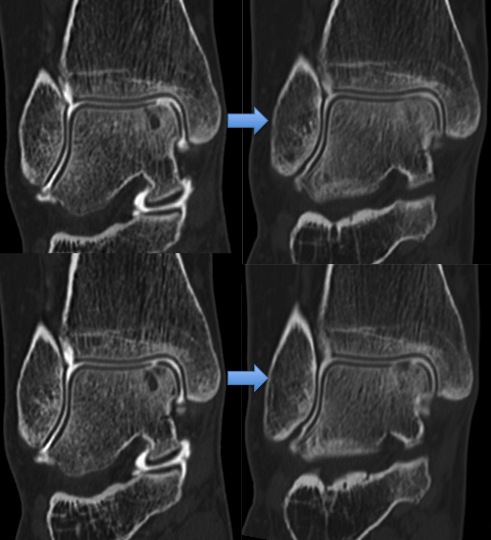
- Open chirurgie (arthrotomie of osteotomie): Le principe est similaire à la précédente à l’exception de l’abord arthroscopique.
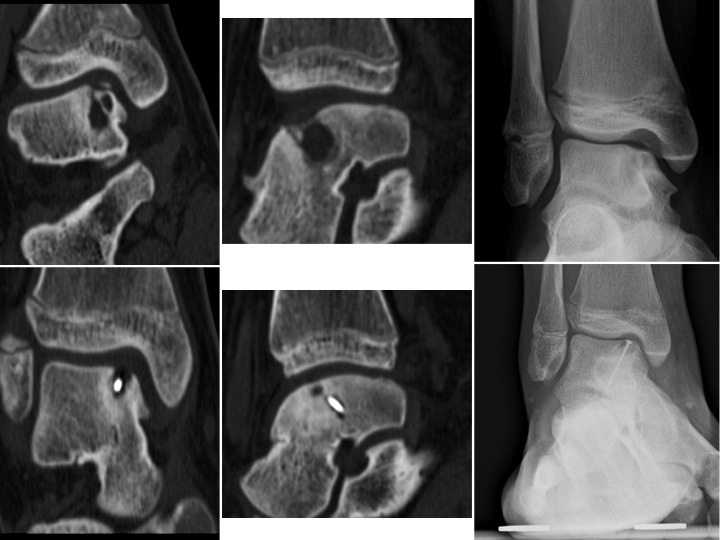
- La greffe ostéochondrale: Elle peut être prélevée soit sur votre genou, soit à partir du matériel synthétique, soit provenir d’une banque d’os. Comme pour l’arthroscopie, là aussi le taux de réussite « n’est que 85% ». Dès lors, on commencera toujours avec une arthrosocopie.
- Allogreffe massive: En cas de kystes volumineux, le remplacement d’une partie de l’os par un os donneur est recommandable.
En cas de fracture non déplacée, une décharge de 6 semaines est de rigueur. Vu le risque possible de lésions fragmentaires, un plâtre plus ou moins amovible durant quelques semaines est à recommander, accompagné d’éventuels exercices de mobilisation par un kinésithérapeute.
En cas de lésion cartilagineuse avec arrachement d’une partie de l’os sous-jacent qui se serait déplacée dans l’articulation, le traitement dépendra du volume du fragment. Si ce fragment est trop petit pour être refixé, on peut simplement l’enlever sous arthroscopie en associant un débridement et des micro-fractures au site de la lésion. En cas de fixation, la situation est comparable à celle d’une fracture non déplacée.
L’ostéochondrite disséquante est une lésion ostéochondrale qui apparaît durant la croissance. Un traumatisme, spontané ou non, peut mobiliser ce fragment, et provoque une inflammation de cette lésion. Le traitement qu’on propose sera:
- Des perforations rétrogrades de la lésion, pour obtenir sa fixation et sa consolidation.
- Une arthroscopie ou chirurgie ouverte avec débridement et micro-fracture.
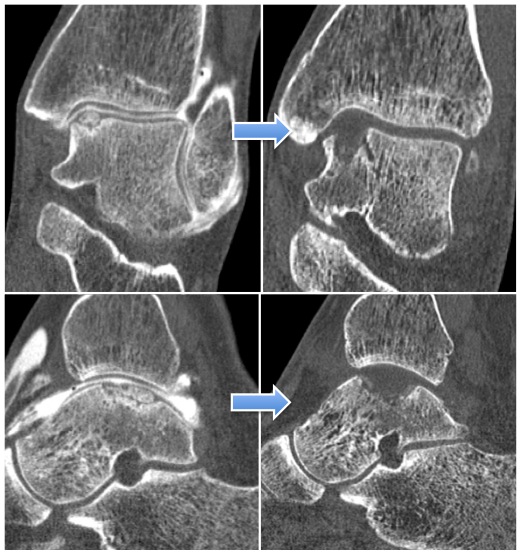
Si l’atteinte du cartilage est étendue et globale dans une articulation, on parle d’arthrose. (chapitre arthrose).

